Hyperparathyroidism Diagnosis
Hyperparathyroidism (HPT) often presents vague symptoms that can occur with other diseases and conditions, so parathyroid disease diagnosis often requires laboratory tests. A Canadian osteoporosis study showed that 1.4% of the population had typical HPT with high levels of calcium and parathyroid hormone (PTH), which is relatively easy to diagnose. However, another 3.3% of the population had normocalcemic HPT, which means they had normal calcium levels and elevated PTH levels.
This group of patients is often misdiagnosed because their calcium level is in the normal range, and routine testing does not account for PTH. As a result, their disease will continue to progress until they develop more severe symptoms, including kidney stones or osteoporosis. The disease entity “normocalcemic hyperparathyroidism” was officially recognized in 2008; yet today, most physicians have still not been taught about it.
The key to making the proper parathyroid disease diagnosis (HPT or any form of it) is to look at the relationship between calcium and PTH in blood tests. In a person who has normal parathyroid glands, when the calcium is low (low end of normal), the PTH will be high (high end of normal) because PTH causes calcium to be released out of the bones and reabsorbed from the urine in the kidneys, and vitamin D is activated to help absorb calcium from food. When the calcium level rises, the parathyroid gland shuts down, and the PTH level goes down because there is no further need for calcium to be taken out of bones and urine. Below are some detailed diagrams about the different forms of the disease.
Normal Parathyroid Glands
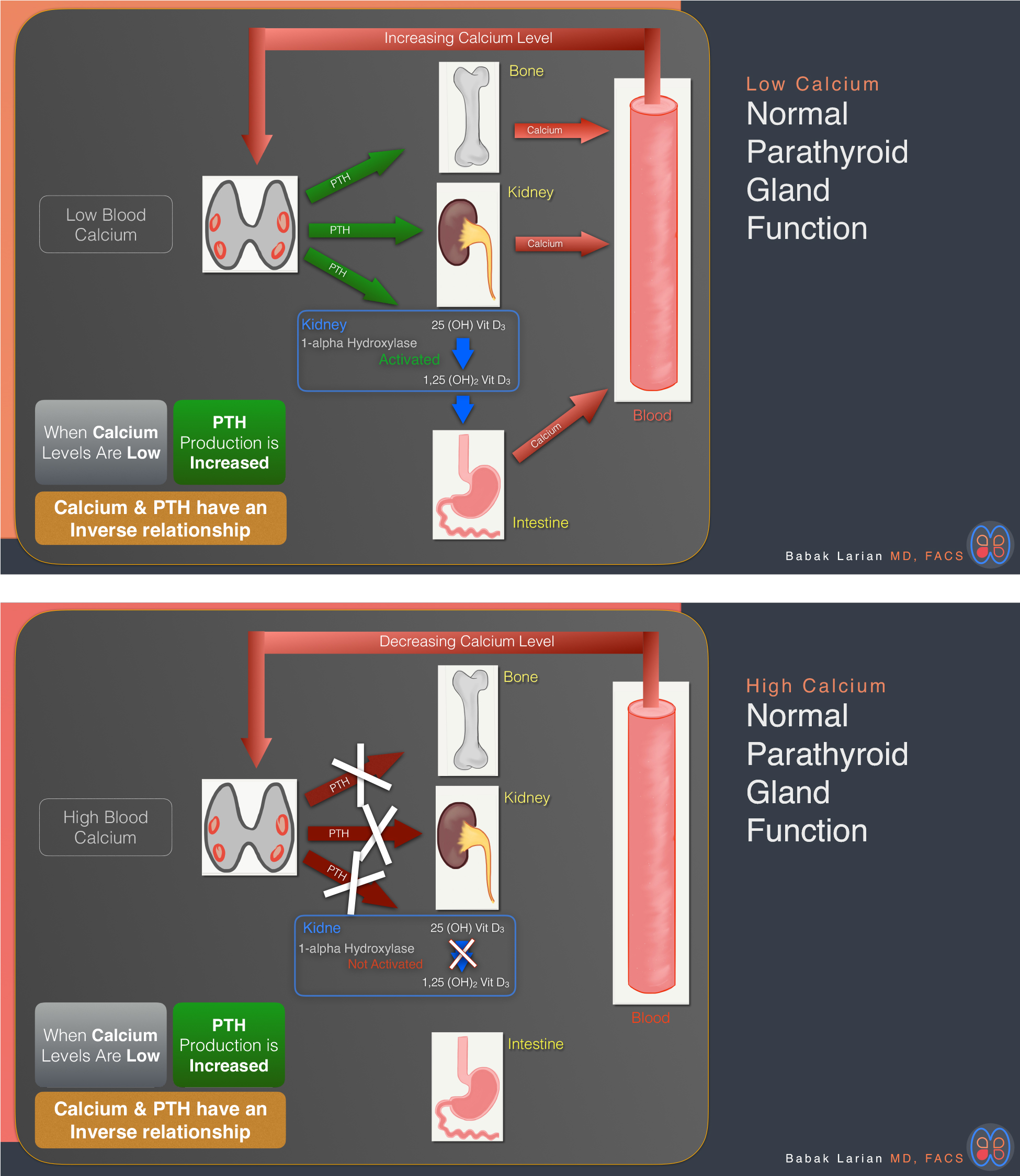
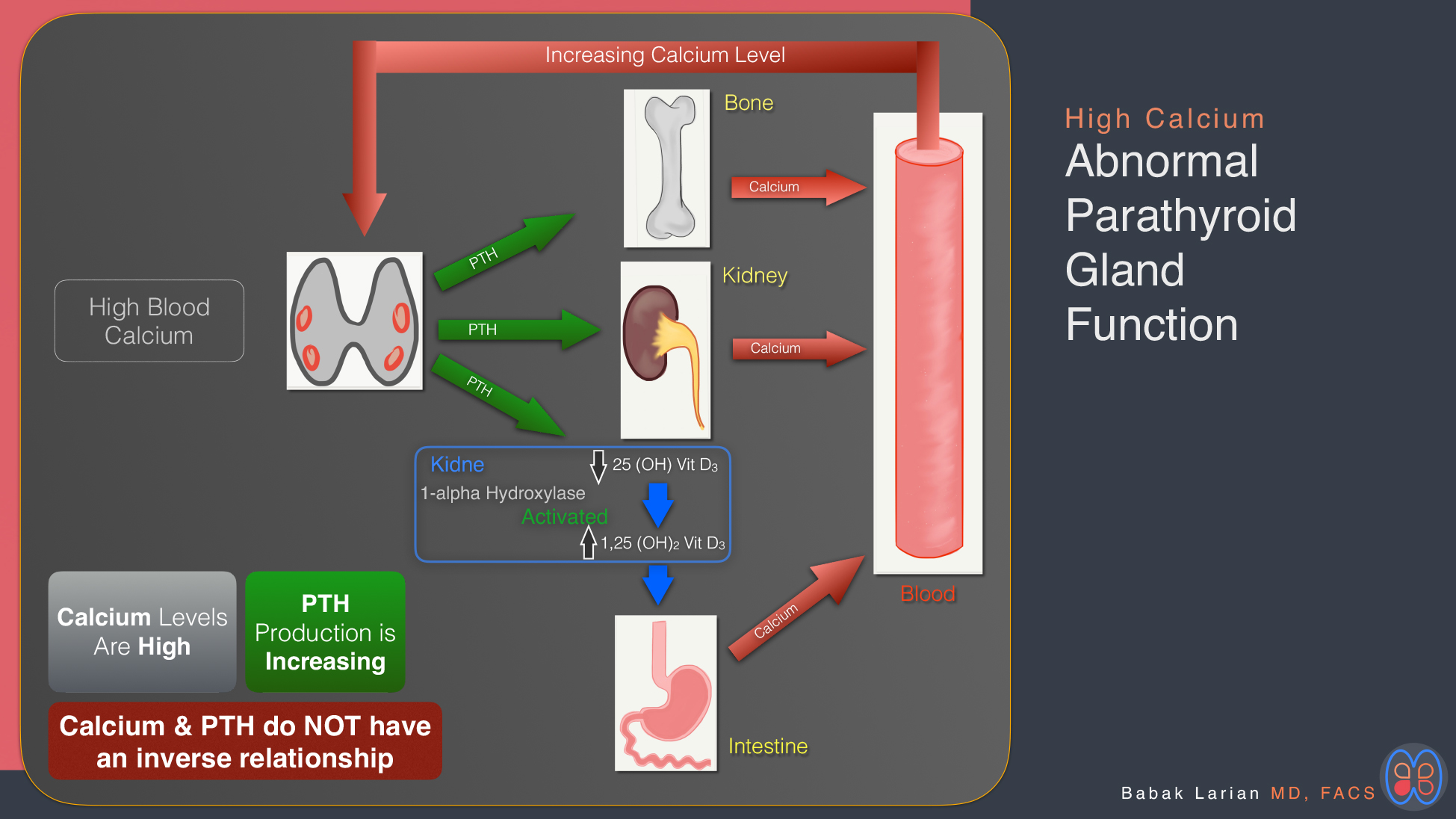
Abnormal Parathyroid Glands
The situation is different in a person that has an abnormal parathyroid gland; the calcium level will be high or high-normal, and the PTH level will be high or high-normal as well. In this situation, the relationship between calcium and PTH is not inverse. In the diagram below, you’ll see that although there is a high blood calcium level, the parathyroid glands are still producing PTH, which is going into the bones and releasing calcium (in time leading to osteoporosis and bone fractures). PTH is also traveling into the kidneys, leading to more calcium collecting in the kidneys (leading to kidney stones) and many other problems.
Furthermore, here is a chart to explain the different presentations of the disease
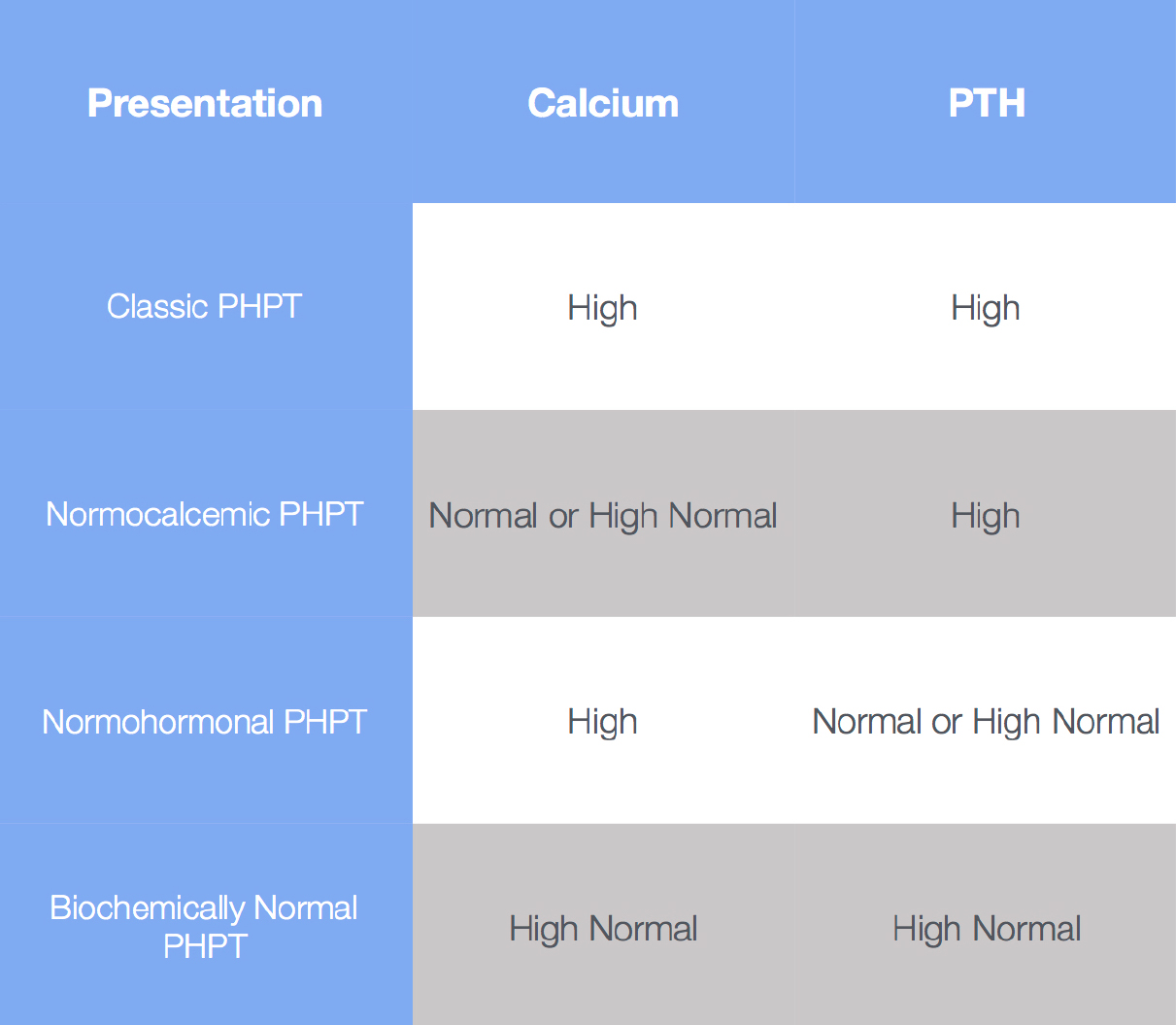
Normocalcemic Primary Hyperparathyroidism
The majority of patients living with normocalcemic primary hyperparathyroidism (PHPT) go undiagnosed for years because they have normal or high-normal calcium levels, even though their PTH levels are above normal.
Normohormonal Primary Hyperparathyroidism
Patients with normohormonal PHPT have high calcium levels but normal or high-normal PTH levels. Many of these patients go undiagnosed because their doctors assume that since their PTH levels are in the normal range, there is no way they have hyperparathyroid disease. But that is false. Patients with these levels can in fact be suffering from HPT!
Parathyroid Disease Case Studies
Below are four examples of patients with parathyroid disease who were diagnosed and treated at the CENTER for Advanced Parathyroid Surgery. You can see that each patient presented HPT with unique symptoms and lab results. A parathyroid disease expert like Dr. Babak Larian is needed in these cases to properly diagnose patients, especially with the “non-textbook” presentations of the disease.
Case Study 1


Case Study 2


Case Study 3

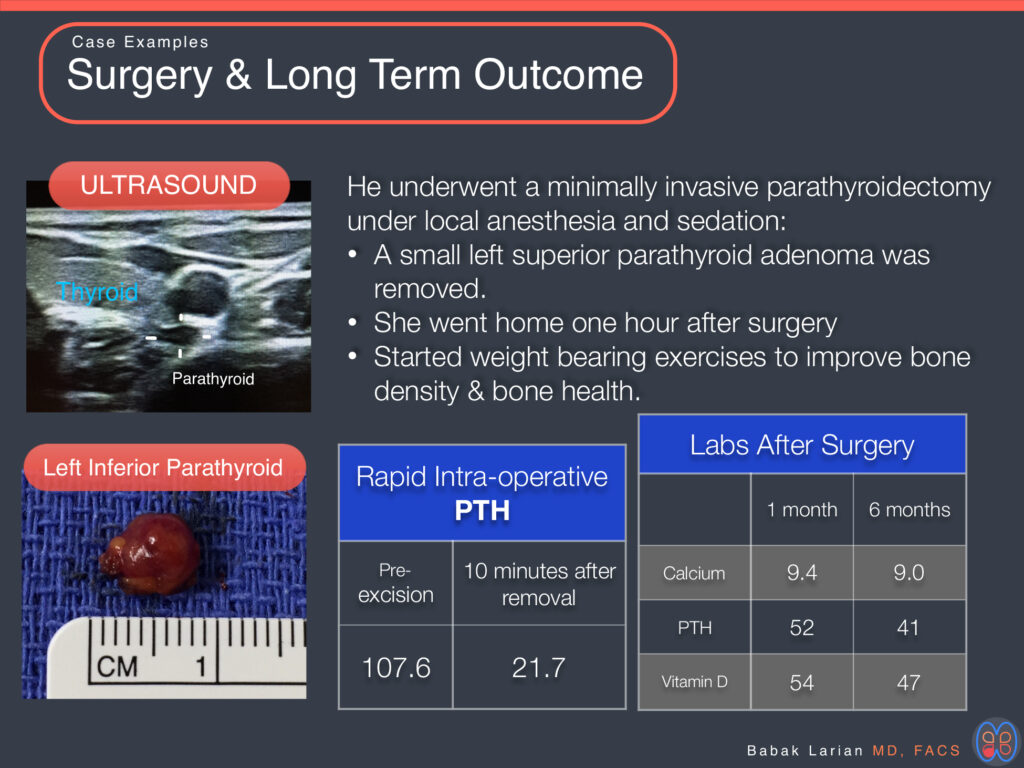
This patient underwent a workup for a wrist fracture. The extent of the fracture in his wrist was disproportionate to the impact (playing with his 2-year-old child). The bone density scan (DEXA) showed he had osteoporosis and severe thinning of the bones in multiple areas. As part of the workup for early onset osteoporosis, he had an elevated PTH level that remained high on repeat testing, and his calcium was always in the normal range. Over the years, his calcium had been checked on his annual exam and blood tests, but because it had always been normal, the PTH level was not checked. Also, his other parathyroid symptoms had been vague and non-specific. He was referred to the CENTER by his endocrinologist for a surgical cure. After surgery, he gradually increased his use of weight-bearing exercises to strengthen his wrist. He repeated the DEXA scan a year later, which showed significant improvement in bone density.
Case Study 4

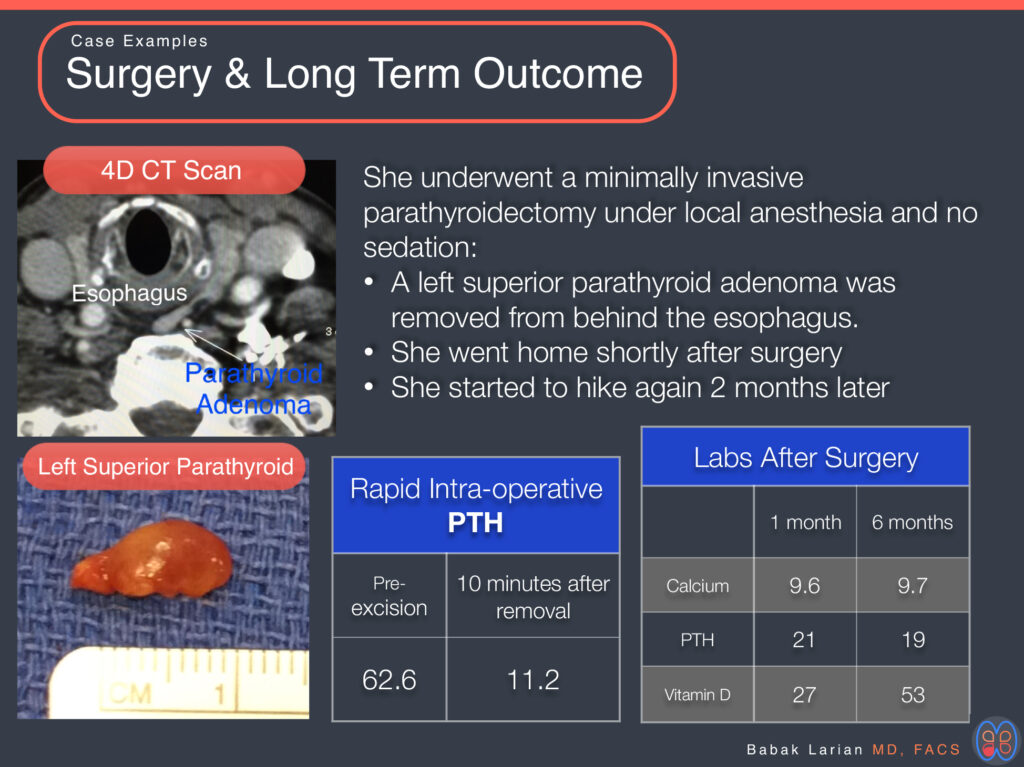
This patient displayed a slight elevation in calcium levels for years and what always seemed to be a normal PTH level (although the PTH level was never on the low end of the normal range). Due to frustration with not having a diagnosis and feeling that her symptoms were progressing disproportionately to her age and generally feeling “something was wrong,” she came to the CENTER. We looked at all her labs over the years and discovered that there was no suppressive relationship between her calcium and PTH levels. We also did further testing to make sure that no other causes of high calcium levels were present. Afterwards, she had a negative ultrasound, and because her PTH was low, we chose to have a 4D parathyroid CT scan, which identified the abnormal parathyroid gland.
How to Diagnose Hyperparathyroidism
HPT diagnosis varies based on a patient’s parathyroid disease symptoms, the severity of these symptoms, and other factors. With support from a parathyroid gland expert like Dr. Larian, anyone can receive an accurate HPT diagnosis and take steps to treat his or her parathyroid disease symptoms.
Dr. Larian understands there is no one-size-fits-all approach to HPT diagnosis. Thus, Dr. Larian personalizes HPT diagnosis and ensures that each patient receives comprehensive testing.
As Dr. Larian conducts HPT assessments, he learns about his patient and tries to identify the root cause of the patient’s symptoms. If Dr. Larian believes a patient is dealing with one or more abnormal parathyroid glands, he may then recommend surgery. At this point, Dr. Larian explains how parathyroid surgery is performed, responds to his patient’s surgery concerns and questions, and prepares a surgery plan.
Primary Hyperparathyroidism Diagnosis
PHPT begins in the parathyroid glands, and it is diagnosed via blood tests to analyze a patient’s calcium and PTH levels. Additionally, a patient may require 24-hour urine collection to test for PHPT; this allows a doctor to test a patient’s urine for the presence of calcium, creatinine, and other waste products commonly removed by healthy kidneys.
The results of PHPT testing are generally sent to a laboratory for analysis. They allow Dr. Larian to see if HPT is caused by a kidney disorder. Also, the tests help Dr. Larian determine if HPT occurs due to hypocalciuric hypercalcemia, a genetic disorder that causes elevated calcium levels in the blood.
Secondary Hyperparathyroidism Diagnosis
Secondary HPT is usually caused by kidney failure; it occurs if the kidneys are unable to remove phosphorus from the body and cannot produce a sufficient amount of vitamin D. Tests may be used to assess a patient’s vitamin D levels, bone mineral density, and urine calcium levels. With this information, Dr. Larian can determine if a patient is dealing with secondary HPT and provide proper diagnosis and treatment.
Symptoms List for Hyperparathyroidism Diagnosis
In order to be able to diagnose a person with hyperparathyroidism, looking at the whole person, and what is happening to them is very important. Going through the symptoms they are experiencing and the impact of those symptoms on their life can give not only help the doctor with the diagnosis, but also figure out the how severely hyperparathyroidism is affecting the person. This information will play an important part in deciding to treat or not, what course of treatment to chose, and if surgery is appropriate when to do the surgery.
Lab Tests for Hyperparathyroidism Diagnosis
Dr. Larian will order the following laboratory tests to help him diagnose hyperparathyroid disease:
- Blood calcium and ionized calcium on two separate occasions (which can be done as little as one week apart)
- PTH (intact) levels on two separate occasions (which can be done as little as one week apart)
- Vitamin D levels, specifically 25 (OH) Vitamin D and 1,25 (OH) vitamin D
- Magnesium and phosphorus levels (to see the chemical balance in the body)
- Basic chemistry and creatinine levels (to assess kidney function)
- Alkaline phosphatase (to check if bone disease is causing the calcium level to rise or the impact of hyperparathyroidism on the bones)
- 24-hour urine calcium and creatinine to assess the degree of calcium loss in the kidneys and help identify familial hypocalciuric hypercalcemia
- Fatigue
- Poor Concentration
- Memory Loss
- Sleep Problems
- Anxiety
- Irritability
- Depression
- Headaches
- Bone Pain
- Osteoporosis
- Joint Pain
- Muscle Weakness
- Bone Fractures Easily or Frequently
- Constipation
- Nausea
- Abdominal Pain/Acid Reflux
- Weight Loss
- Kidney Stones
- Frequent Urination
- Night-time Urination
- Urinary Incontinence
- High Blood Pressure
- Heart Palpitations
- Hair Loss
In normal functioning parathyroid glands, if the blood test indicates too much calcium is present in the blood, the PTH levels should be low (or suppressed) so that the body has a chance to bring the calcium back down to a normal level. If this suppressive pattern is not present and on two separate occasions the blood tests show a calcium and PTH imbalance, then the HPT diagnosis is confirmed. Oftentimes at the CENTER, we will have to repeat the laboratory tests to both confirm the diagnosis of HPT and look at all other possible diseases that can cause a calcium imbalance.
If the blood test indicates excessive calcium in the blood AND a high level of PTH (not a suppressed parathyroid gland), Dr. Larian can draw the conclusion that the parathyroid gland is not functioning properly and HPT is present.
The most important thing to understand in terms of diagnosing hyperparathyroid disease is that just because you don’t have the “normal” presentation of the disease does not mean you do not have parathyroid disease! Every patient has a unique presentation of the disease and should be evaluated on an individualized basis. You do not need to have both high PTH and high calcium levels in order to have the disease.
Vitamin D and Hyperparathyroid Disease
Normal vitamin D levels in adults are between 30 and 100 ng/mL. Vitamin D helps our intestines
absorb calcium from the food we eat, as well as helps our bones reshape themselves and grow stronger. Vitamin D has many other important functions,
A low vitamin D level is common, even in healthy people. It is especially common in people with HPT; it’s found in about 80% of patients who have high blood calcium and PTH levels. There are two possible reasons for this phenomenon:
1. Secondary Hyperparathyroidism Due to Vitamin D Deficiency
If a person has a vitamin D deficiency, it can secondarily cause an elevated PTH level, which may cause the calcium level to increase as well. These patients generally have normal or slightly elevated calcium levels, and when the vitamin D is replenished and comes back to normal levels, the PTH and calcium levels return to normal levels.
2. Low Vitamin D Level Due to Altered Vitamin D Metabolism
When calcium rises in HPT, the body is not able to decrease the calcium level in the blood. This occurs due to the fact that the parathyroid glands control the blood calcium level, and now that they are malfunctioning, the calcium level stays up. It has been theorized that since the abnormal parathyroids cannot be controlled to bring the calcium level down, the body tries to decrease its vitamin D levels to reduce calcium absorption from foods. In this group of patients that have PHPT, vitamin D replacement does not correct the PTH and calcium imbalance, and it may also make them feel worse than ever before. These patients feel especially bad, even if they are given a high dose of vitamin D weekly.
However, many adults are vitamin D-deficient but do not have parathyroid disease. Vitamin D deficiency can occur as a result of poor diet and/or not spending enough time outdoors. In these cases, people simply need to take a vitamin D supplement to return their vitamin D levels to the normal range in order to maintain good health and bone calcium.
Scans to Locate Parathyroid Tumors
- Ultrasound: Uses soundwaves to examine the parathyroid glands, blood vessels, and other structures under a patient's skin.
- Sestamibi Scan: Uses a radioactive dye to help a doctor identify a malfunctioning parathyroid gland.
- SPECT: Uses 3D images to pinpoint the location of an enlarged parathyroid gland. Usually combined with the Sestamibi Scan.
- 4D Parathyroid CT Scan: Uses the difference in absorption of iodine contrast at different times after the injection to identify an enlarged active parathyroid gland.
One or more of the aforementioned tests may be used to determine the location of an abnormal parathyroid gland. Additionally, a 4 gland assessment and intra-operative PTH testing may be required before parathyroidectomy surgery is performed.
I traveled from Washington DC to Los Angeles to have Dr. Larian perform my recent parathyroidectomy. I struggled unsuccessfully for months to find a local surgeon who could diagnose my hyperparathyroidism, and was fortunate enough to learn about Dr. Larian while doing my own research. Few doctors are knowledgeable about parathyroid disease, even fewer can perform the surgery successfully using minimally invasive procedures. After years of vague symptoms and months of severe symptoms, just days after surgery I feel better than I have in such a long time.
FAQ (Frequently Asked Questions)
- Can a single test be used to diagnose hyperparathyroidism?
In certain cases yes; that is when calcium is very elevated and PTH is clearly high. An example is when the calcium is 11.8 mg/dl & PTH is 210 pg/ml.
But not all cases have clear numbers, so in most of the cases getting more then one set of labs is helpful to confirm the diagnosis (meaning getting labs done on 2 separate occasions, that can be as early as one week apart). Accuracy is key, especially when it comes to HPT testing.
- How many tests are required to properly diagnose hyperparathyroidism?
The number of tests required to diagnose HPT varies based on the patient. Dr. Larian’s goal isto provide each patient with an accurate diagnosis. Some patients have a clear laboratory presentation of hyperparathyroidism (textbook cases) and may need one set of labs; others may have more complex issues and require multiple sets of labs and replacement of minerals and vitamins before the picture becomes more clear.
To accomplish his goal, Dr. Larian will assess each person individually, conducts the necessary testing and analyzes the test results, he then provides a diagnosis and treatment plan.
- What is the best test to diagnose hyperparathyroidism?
There is no surefire test that determines if a patient is dealing with HPT. Instead, several tests are often used to ensure a patient receives an accurate diagnosis. For example, blood tests are frequently used to assess a patient’s calcium, PTH and Vitamin D levels. Other blood tests may be used to analyze a patient’s phosphate, magnesium, creatinine, and alkaline phosphatase levels. Meanwhile, a urine test may be required to evaluate the amount of calcium in a patient’s urine over a 24-hour period.
- When is the best time to do blood tests to diagnose hyperparathyroidism?
It is best to do blood test for HPT first thing in the morning before eating anything. This is called a fasting blood test. Doing it this way will minimize the impact of food or activity on calcium and PTH levels.
- How much time is required to undergo testing for a hyperparathyroidism diagnosis?
Some tests require only minutes to complete, but it may take a few days before the test results become available. Dr. Larian explains all aspects of HPT testing before any assessments are performed. This ensures that a patient knows how much time is required for each test, when is the best timing to do the test, as well as what to expect during and after each assessment.
- Is testing for hyperparathyroidism safe and effective?
HPT diagnosis is most often accomplished through blood & urine testing. These tests are relatively simple and without risk.
- What information does a 24 hour urine calcium test give?
The 24 hour urine calcium test shows how much calcium is being released by the kidney into the urine. The kidney is the main filter for calcium, so if your blood calcium level is high, the kidney is going to try to get rid of the excess calcium through the urine. If you have high blood calcium levels, but the amount of calcium in the urine is very low, then you have to look at thekidney to see if that is the source of the problem.
A condition called FHH (Familial Hypocalciuric Hypercalcemia) can cause the kidney to filter only very small amounts of calcium, and in turn cause the person to have high blood calcium levels. A person with FHH is not ill and has no symptoms; the body being so incredible, from birth compensates and learns to adjust to the kidney issue. The diagnosis is made initially by seeing low levels of 24 hour urine calcium, which jcan be confirmed by seeing the comparison of how the kidney filters calcium as compared to other compounds (creatinine). If that shows that the comparison is very low then we the diagnosis is usually confirmed by doing genetic testing. These patients do not need or benefit from surgery.
Rarely, this condition can be present at the same time as hyperparathyroidism, making the diagnosis of hyperparathyroidism very challenging.
- When should a 24 hour urine calcium test be done?
If calcium levels are slightly elevated but the PTH is not high, a 24 hour urine calcium is done to see if the rise in calcium is caused by FHH or by the parathyroid (normohormonal hyperparathyroidism).
When doing this test, it is best to get the urine collection bottle from the laboratory first. Start collecting urine in the morning and continue till the following morning. Then deliver the urine on the second morning, DO NOT HAVE BREAKFAST, and also do your blood test checking calcium, PTH and Vitamin D (and others ordered by your doctor) on that morning while you are fasting. This will give you the most accurate results.
- What information does a PTHrp test give?
PTHrp or Parathyroid Hormone related peptide, is a hormone that is produced by the placenta and certain cancers (Breast cancers and some lung cancers, among others). PTHrp acts like PTH and cause calcium levels to rise.
So if a person has high blood calcium levels and low PTH levels, one must look at PTHrp among other labs to make sure the elevation in calcium is not being cause by the hormone PTHrp produced by the cancer. If PTHrp is high then the person does not have Hyperparathyroidism, and if they are not pregnant, then thorough search for a possible cancer must be undertaken.
- What information does a ACE test give?
ACE levels can be elevated in a condition called sarcoidoisis. This is an inflammatory condition that causes collection of inflammatory cells that create a compound that is similar to vitamin D, this in turns increases absorption of calcium from the gut, and cause calcium to go up.
Most but not all these patients will have these pockets of inflammation in the lungs, so a chest xray or chest CT scan will help with diagnosing this condition.
- Why should I choose Dr. Larian for hyperparathyroidism testing?
Dr. Larian is a parathyroid surgery expert who understands what it takes to properly diagnose and treat HPT symptoms. For many years, Dr. Larian has helped patients uncover the root cause of their HPT symptoms. He works diligently to assist his patients, and with HPT testing, enables patients to achieve long-lasting HPT symptom relief.
Speak With Parathyroid Specialist Dr. Larian Today
If you have been living with the signs and symptoms of hyperparathyroid disease, it is time to be properly diagnosed! At the CENTER, you are in great hands than with our parathyroid specialist.
Dr. Larian treats every patient on an individualized basis, and his top priority is curing your disease. To schedule a parathyroid disease diagnosis and treatment consultation with Dr. Larian, please contact us online or call us today at 310-461-0300.
