HPT Testing: Everything You Need to Know About Rapid Intraoperative PTH Assessments
Our philosophy at the CENTER for Advanced Parathyroid Surgery is to be as thorough and comprehensive as possible. Traditionally, parathyroid surgery was difficult to perform, and it was challenging to achieve the desired surgery results due to the following factors:
- Before going to surgery, the surgeon not knowing exactly which parathyroid gland and how many parathyroid glands are abnormal.
- All four glands being found and biopsied.
- All four glands being looked at and compared under a microscope to see which
glands appeared normal and which ones appeared to be abnormal (an unreliable
method of assessing parathyroids).
This invasive approach to surgery resulted in high complication rates and inconsistent outcomes. This is why Dr. Babak Larian has continued to stay on the cutting edge of science & technological advances to improve treatment of hyperparathyroidism. Today, Dr. Larian utilizes a minimally invasive approach to cure hyperparathyroidism (HPT); this means that during surgery he only finds and removes the abnormal parathyroid gland, and does not disturb and impact the normal parathyroid glands. The notion of minimally invasive surgery is depends on the fact that the surgeon should not disturb areas, organs, glands that are healthy and should be allowed to fully function for the person. This was not achievable in the past because of the need to find all four glands to either visually decide or use radioguidance to decide which parathyroid gland is abnormal.
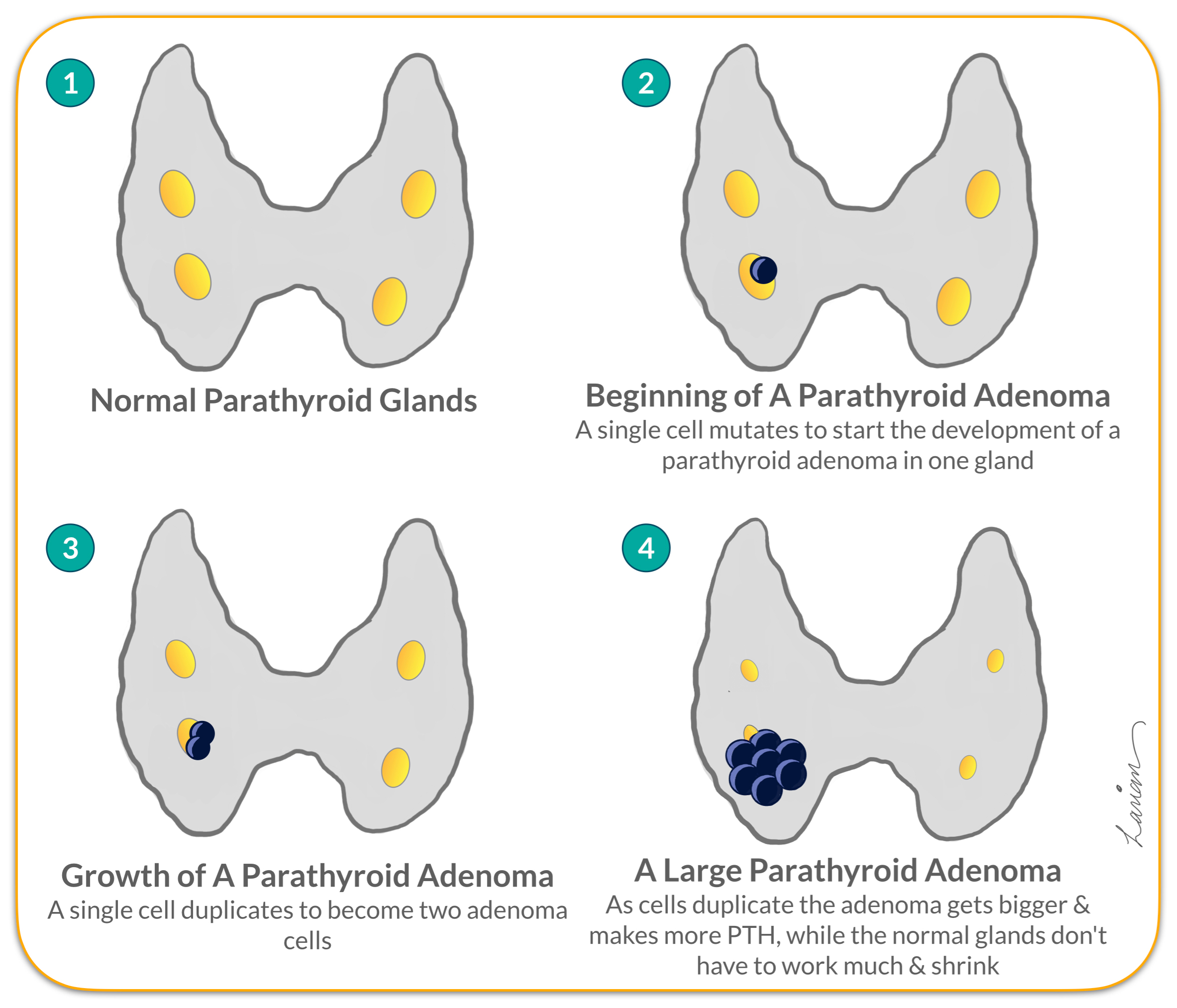
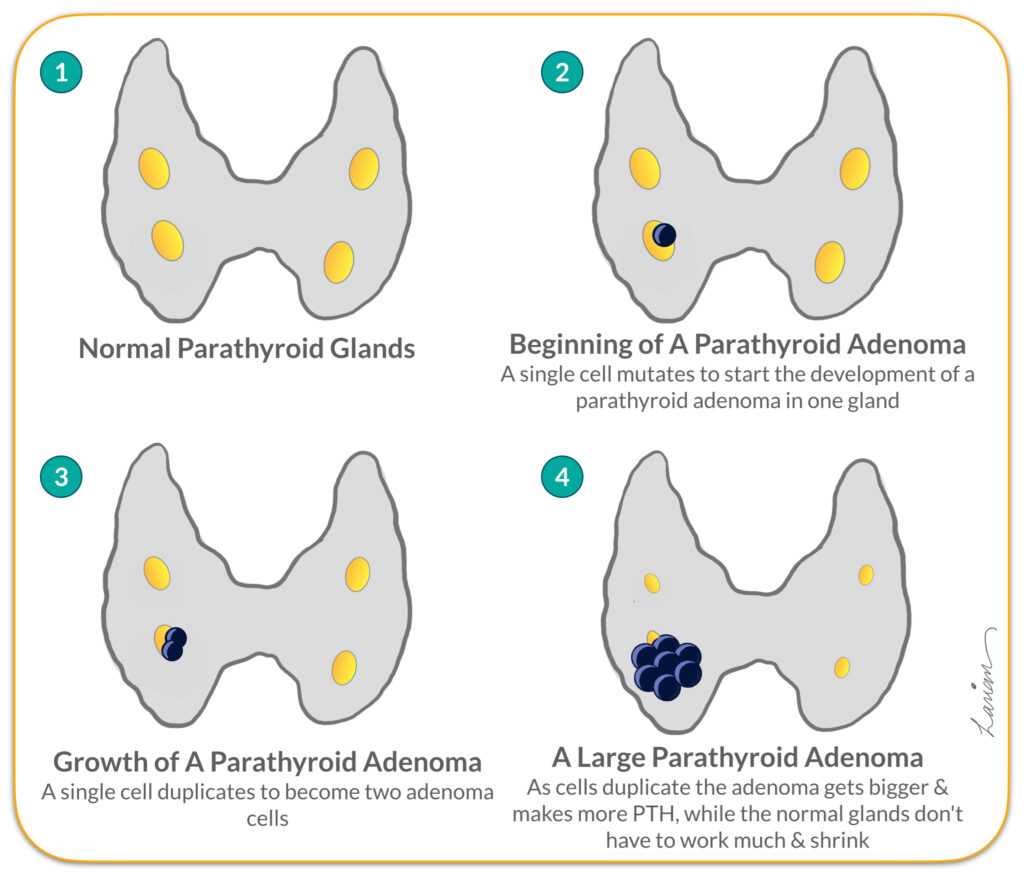
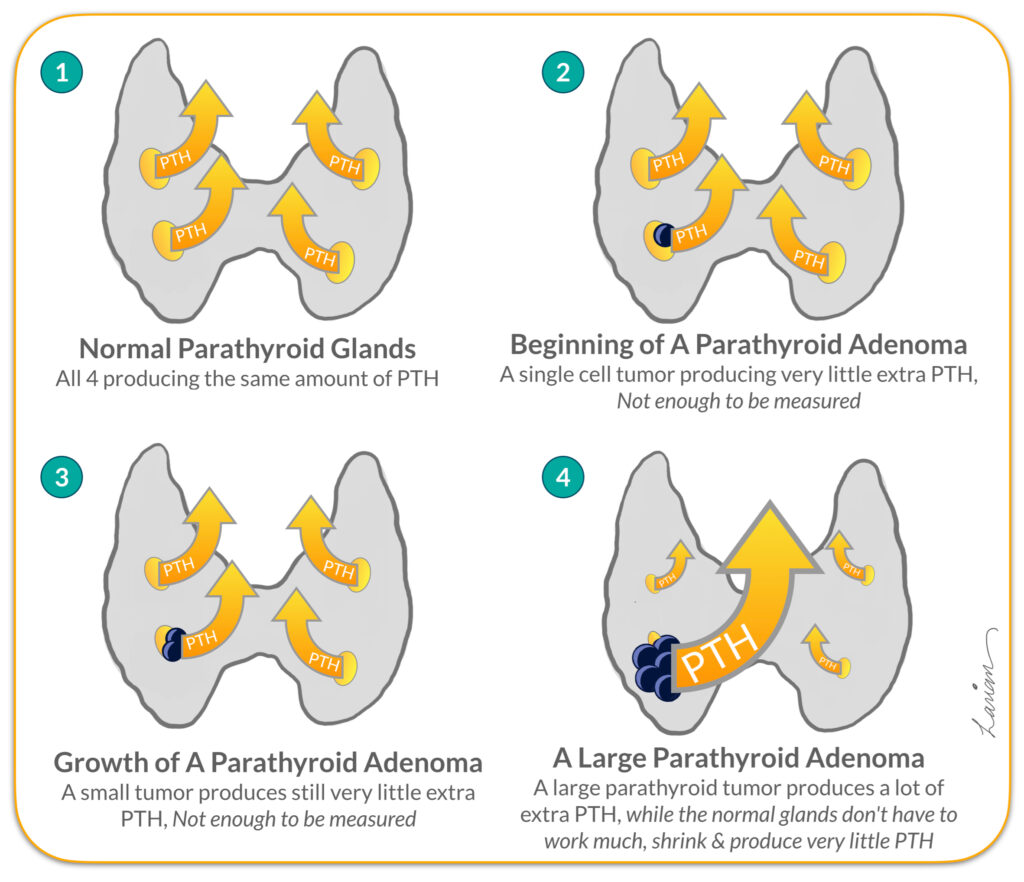
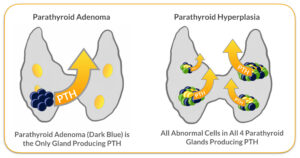
The problem with these maximally invasive parathyroidectomy procedures is that when a parathyroid tumor develops the remaining glands that are not working shrink and get smaller (diagram 4 in the Figure to the right). This is because the body wants parts that are not working to not use energy unnecessarily. Just like a muscle that doesn’t exercise shrinks and gets smaller. Additionally all Parathyroid glands have one blood vessel (artery) coming in that brings nutrition & calcium to the glands, and one blood vessel (vein) that takes PTH away to from the gland to the rest of the body. As the abnormal gland gets bigger the blood vessels get bigger, and the glands that are not working will have blood vessels that shrink along with the glands shrinking.
So when treating hyperparathyroidism caused by a single parathyroid adenoma, the search for the remaining normal can cause damage for the smaller normal sleepy parathyroid glands and their smaller blood vessels. Which could cause permanent hypoparathyroidism. Minimally invasive focused parathyroidectomy with intraoperative PTH testing cannot cause hypoparathyroidism in a person that has one abnormal gland.
The Reason Why Intra-Operative PTH Testing Works
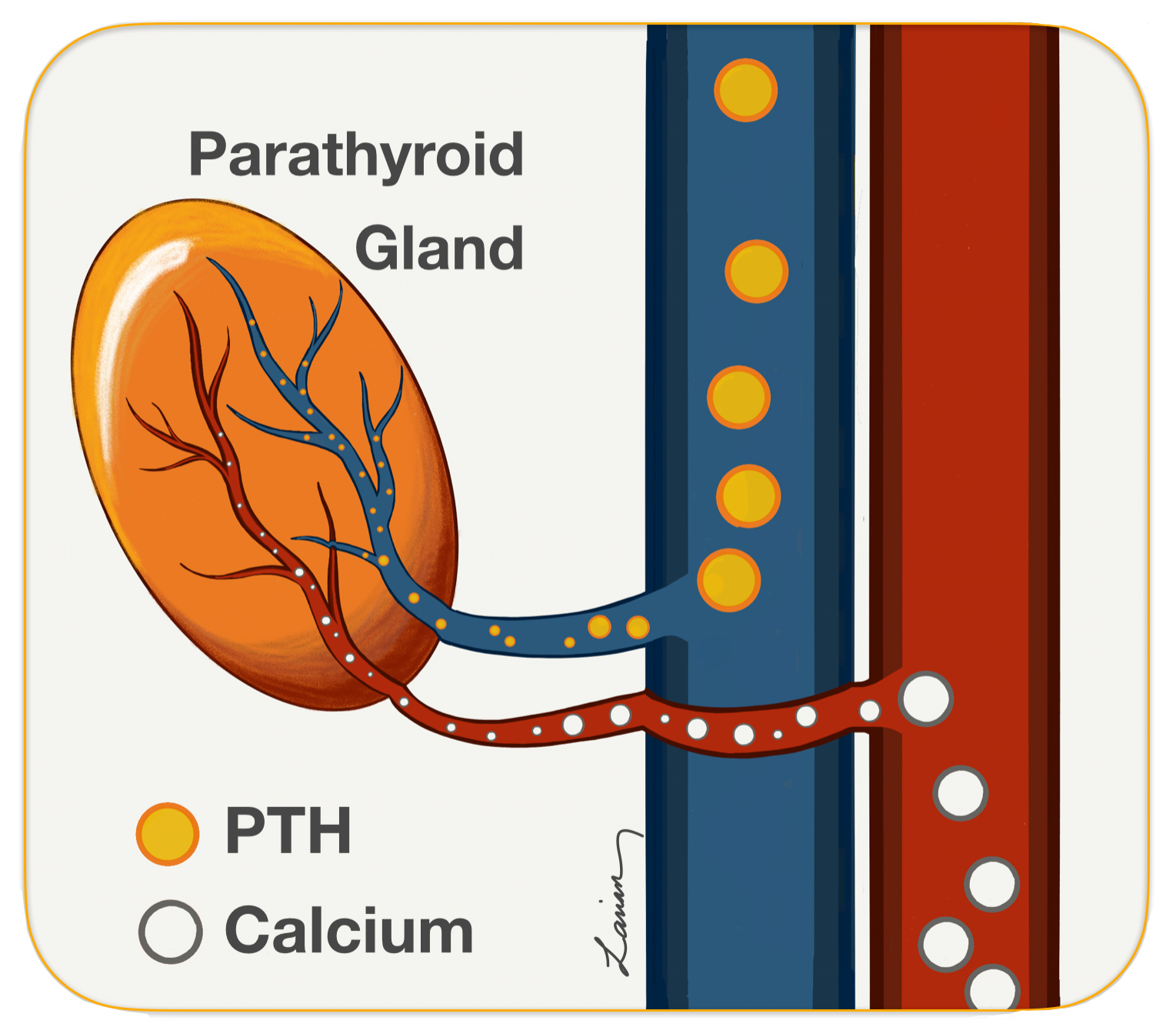
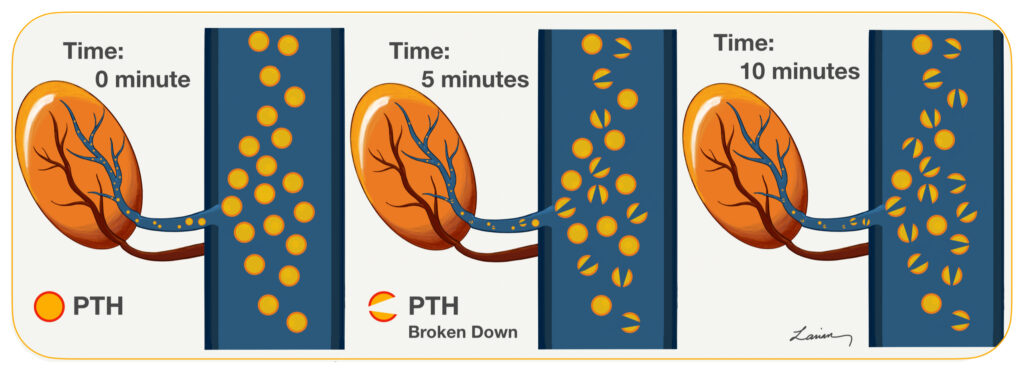
Parathyroid Hormone or PTH is released into the blood by the parathyroid gland in response to low calcium. PTH has a very short half life of about 5 minutes, which means that half of the PTH produced at this moment is broken down and will not work in 5 minutes, by 10 minutes 75% is broken down.
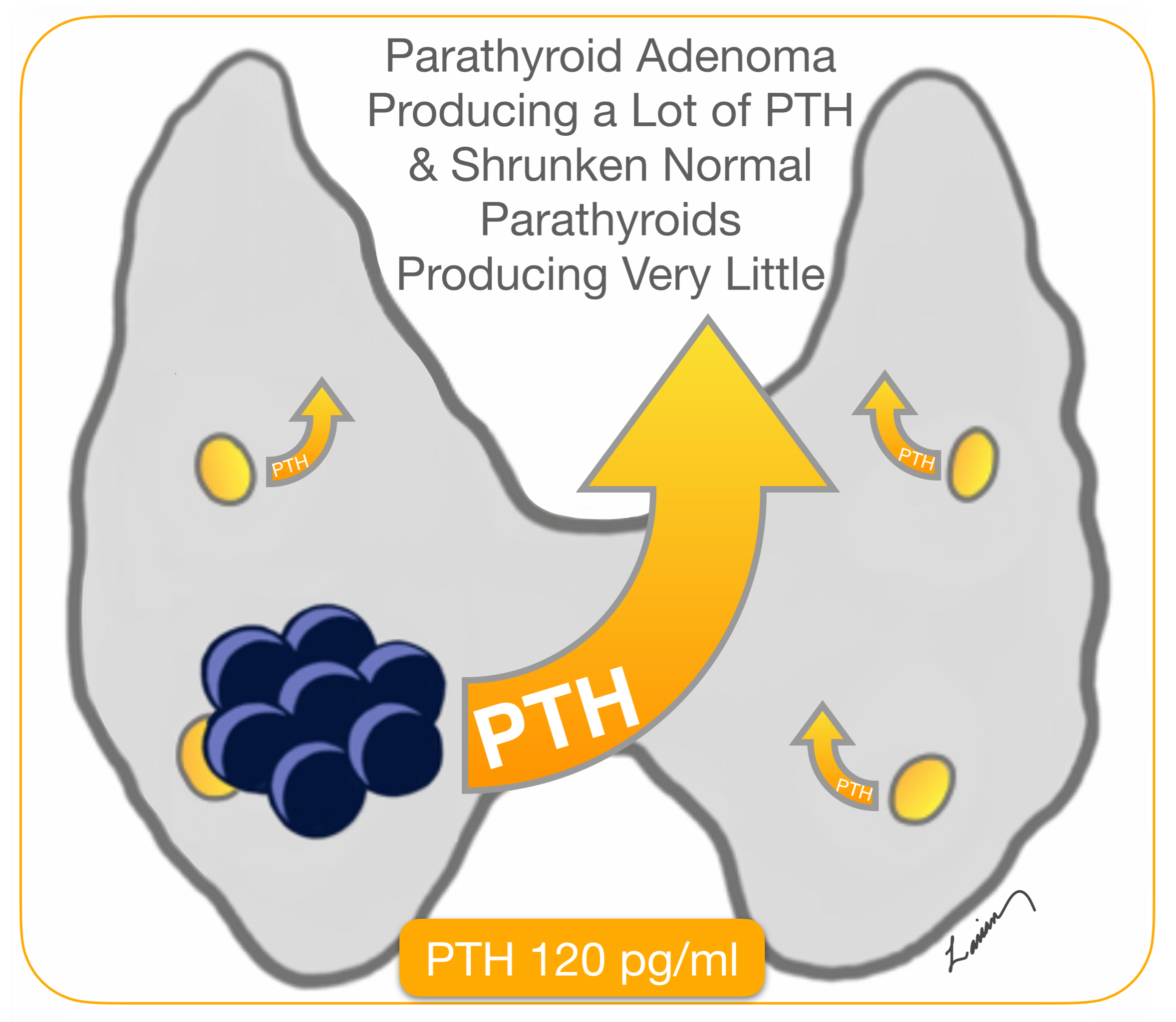
In 1990’s a brilliant physician Dr. George Irvin at the University of Miami realized he could use this information to help in surgery. He understood that when a parathyroid adenoma is working hard and producing a lot of hormone (PTH), then the remaining normal glands would not need to work. These none working parathyroid glands shrink, get smaller (atrophy), and produce very little PTH. When the parathyroid adenoma is removed in surgery, the normal smaller parathyroid glands that have not been doing much work for a long time will still make very little PTH. It takes a few weeks before these normal glands go back to working normally.
The problem had been up to this point that the laboratory test to check for PTH took several hours to days to give results, which made it not useful during surgery. However, Dr. Irvin had at his hospital a rapid PTH machine which he could get results in 30 minutes. This was also a revolutionary change in parathyroid surgery, because with rapid PTH testing you didn’t have to inject a foreign radioactive material to check the level of activity of the parathyroids, but rather the surgeon could just check the amount of PTH hormone being produced during surgery to know if there are still over-active parathyroid glands.
Minimally invasive parathyroidectomy with rapid intraoperative PTH testing was very exciting, because it could truly let surgeons be minimally invasive (meaning in surgery only disturb the abnormal gland), and check how active the other 3 glands were by directly checking the blood levels of PTH, the hormone causing all the problems in hyperparathyroidism. Over time surgeons realized intraoperative PTH testing was even more useful then originally anticipated; not only could the surgeon confirm the the success of surgery once the abnormal gland or glands had been removed, they could also make sure the remaining glands were still working. The combination of minimally invasive parathyroidectomy and intraoperative PTH testing has proven to be very reliable with 99% cure rates being reported with this approach. While at the same time minimizing risks because you explore more then one area only when PTH levels don’t come down appropriately (which happens less then 25% of cases). So the 75% of people who have a single adenoma don’t need to undergo a surgery that risks damage to the nerves, blood vessels, thyroid and parathyroids on both sides.
However, there was a clear limitation to this technology; the rapid PTH testing machine was not available at most hospitals. So most parathyroid surgeons did not have access to it. And it took years for surgeons that were dedicated to doing parathyroid surgery to convince their hospitals to purchase these expensive machines and learn how to use intraoperative rapid PTH testing properly. In my case this happened in 2005. Additionally, it required the surgeon to change the way they performed the surgery: (1) they had to have more exact localization studies then the sestamibi nuclear scan alone to find the enlarged parathyroid gland, and (2) the surgery took longer because they had to wait an additional 30 minutes during surgery to get blood PTH results during which they had to mostly sit patiently to see if the numbers came to down appropriately before they were confident the parathyroid they had removed was the only one that was overworking. Not all surgeons had that kind of patience, and if the PTH level did not come down then they had to continue operating and keep testing which could make the surgery much longer. It required parathyroid surgeons to make a complete shift in the way they did parathyroid surgery.
Minimally Invasive Parathyroidectomy (MIP)
Watch the video below to learn more about how Dr. Larian performs MIP to cure HPT patients.
Intra-Operative PTH Testing FAQ
Parathyroidectomy surgery and associated intra-operative PTH testing are sometimes tough to understand. Fortunately, Dr. Larian prioritizes patient education, and provides answers to some of the most frequently asked questions surrounding PTH testing below.
Yes. Caution is key with parathyroidectomy surgery, and thanks to a PTH blood test, an HPT patient receives assurance that all diseased parathyroid glands were properly removed during surgery. Plus, a PTH test is simple to perform and helps determine if a patient is coping with multiple abnormal parathyroid glands. The surgeon will know before the patient leaves the operating room that the surgery was successful.
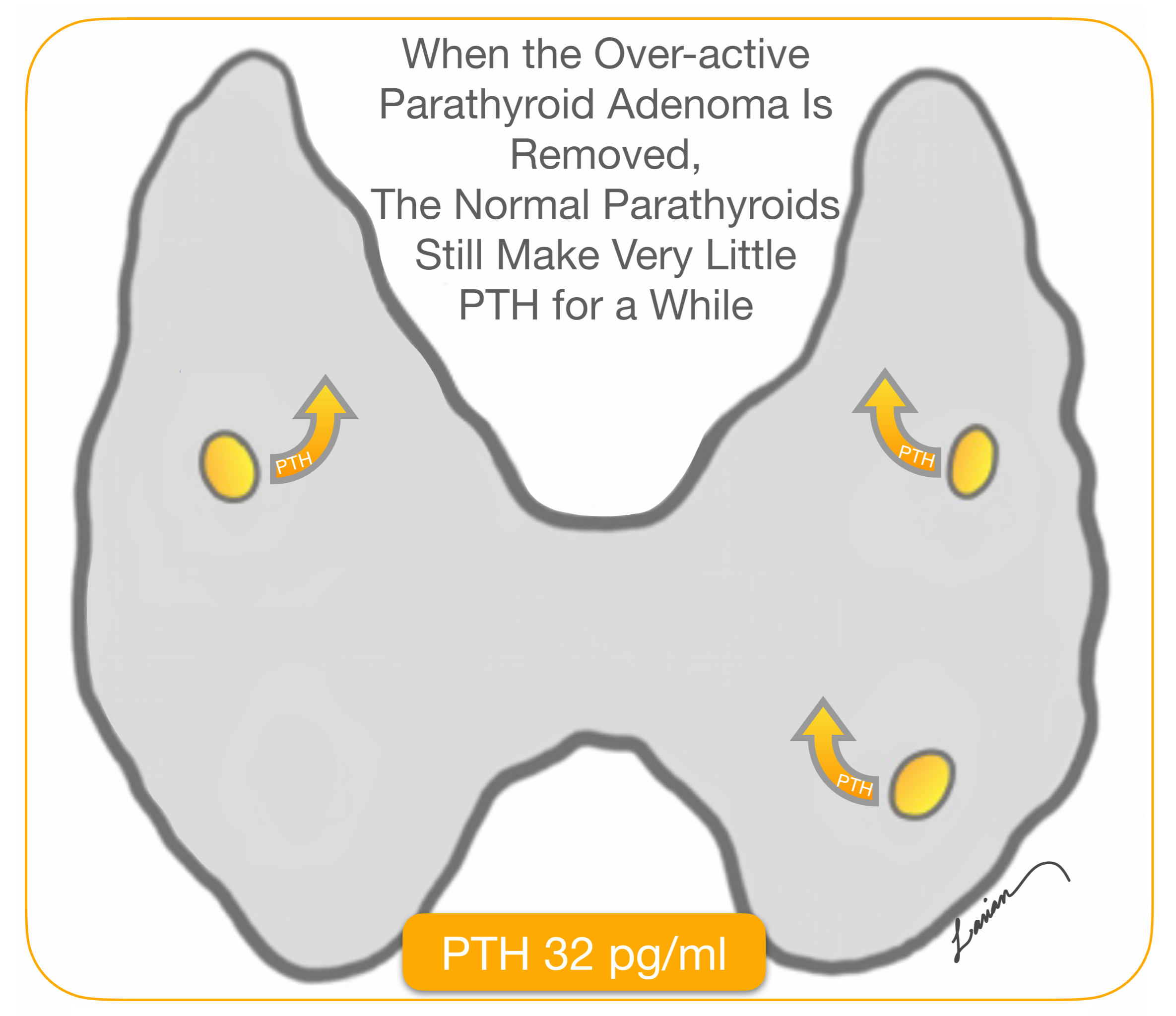
As in the case below, this person had high calcium levels and PTH that was 86 immediately before the surgery started. 10 minutes after the right upper parathyroid adenoma was removed, the PTH level dropped to 32, which is more then the 50% decrease necessary . This shows that the 3 remaining parathyroids are not working much, therefore they are normal parathyroid glands. The surgeon can tell the patient, immediately after surgery, with confidence that the surgery was very successful.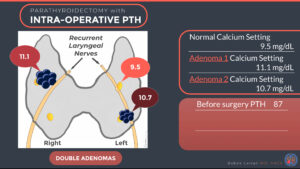
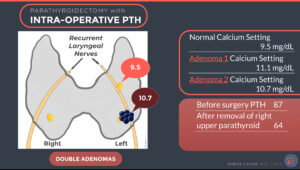
If the patient with hyperparathyroidism has only one parathyroid obvious on a scan (right upper one), and a questionable lesion on another scan elsewhere (left lower), the surgeon would begin by doing a PTH level right before surgery which is 87. After the right lower parathyroid is removed, PTH comes down to 64 which is not an appropriate decrease in PTH if the right lower was the only abnormal parathyroid gland (less than a 50% reduction in PTH). This means that there is another abnormal parathyroid that is producing PTH also. Since a second target had been seen on the localization scan, that was the next parathyroid gland to identify and if abnormal remove. Once the left lower parathyroid was removed, the PTH level done 10 minutes later shows a large drop in level to 16. This means that the other 2 parathyroid glands are normal and not producing too much PTH, and that the surgery was successful. It also means that the right upper and left upper parathyroid do not need to be found and potentially damaged.


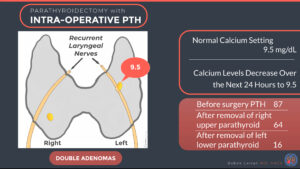
Yes, absolutely. In hyperplasia cases where all 4 parathyroid glands are different sizes, when localization scans are done 1 or 2 of the larger parathyroids may show up on the scan but not the small ones.
CASE: A 43 year old woman with chronic pain and osteoporosis. Calcium levels have slowly been rising up over the past decade, and have been above normal range over the past 4 years. PTH levels are also gradually increasing. Sestamibi and 4D parathyroid CT scans were both negative. Ultrasound done in the office indicated possible enlarged parathyroids in the left upper and right lower areas. She does have a family history of an aunt with untreated hypercalcemia. All together there was a higher degree of suspicion that this may represent parathyroid hyperplasia.
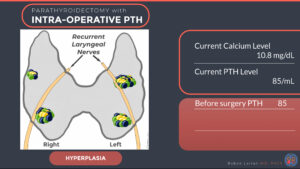
PTH levels obtained before surgery was 82 pg/ml. The left upper parathyroid was to be
identified first as it was the largest on ultrasound and potentially an adenoma. The left recurrent laryngeal nerve was identified and could be seen going over the left upper parathyroid, the nerve was then gently separated from the the parathyroid gland. The left upper parathyroid was clearly enlarged, brownish in color and plump, as such it was removed and PTH levels checked after 10 minutes which showed only minimal reduction down to 67 pg/ml.

The exploration continued and the left lower parathyroid was identified immediately next to the nerve; it was slightly enlarged. Attention was directed to the right side, the lower and upper parathyroids were found after identifying and protecting the voice box nerve (Recurrent Laryangeal Nerve). The right lower parathyroid was similar in size to the parathyroid glands on the left. The right upper parathyroid was much smaller and farther away from the nerve, as such it was deemed to have the lowest growth rate & PTH production; it was biopsied to confirm it was a parathyroid gland. The left lower and right lower parathyroids (that were larger) were also removed and PTH levels tested again; the number came down to 17 pg/ml indicating not only the success of the procedure but the fact the right upper parathyroid was functioning adequately.
The illustration below is the stepwise illustration of PTH drop with every removed hyperplastic parathyroid gland:

VERY IMPORTANTLY, it can tell you how well the last remaining whole parathyroid gland or partially respected parathyroid gland is doing! This is very important because then you know during surgery if you have an adequate amount of functioning parathyroid left behind; this is a very good way to try to minimize the risk of a complication of surgery (permanent hypoparathryoidism).
Localization studies and intra-operative PTH testing are crucial parts of hyperparathyroidism surgery. Yet, these assessments are sometimes ignored as part of the parathyroidectomy treatment process. And in some instances, HPT patients suffer the consequences.
For example, if multiple abnormal parathyroid glands are present but go undetected prior to a parathyroidectomy, a patient is unlikely to know about these diseased glands. As a result, if PTH testing is not completed, a patient may continue to cope with HPT symptoms, even after a parathyroidectomy surgery is completed.
By partnering with Dr. Larian, patients receive personalized support to treat HPT symptoms. First, Dr. Larian helps the patients come to the correct diagnosis, and then conducts the appropriate localization studies to identify any abnormal parathyroid glands. Dr. Larian then offers a custom treatment plan to address diseased parathyroid
glands, which may include parathyroidectomy surgery.
Before Dr. Larian performs parathyroid gland surgery, his patient is prepared for treatment. Dr. Larian teaches his patient about parathyroidectomy surgery and responds to any concerns or questions. Furthermore, Dr. Larian provides post-parathyroidectomy information, so his patient can fully recover from surgery, as quickly as possible.
On the day of a parathyroid gland procedure, Dr. Larian performs rapid intraoperative PTH testing. He ensures that all abnormal parathyroid glands are removed, as well as tracks a patient’s progress following treatment. With this approach, Dr. Larian has become a leader in parathyroid gland surgery.
Talk to a Parathyroid Expert Today!
Dr. Larian offers insights into parathyroidectomy surgery and PTH testing and is happy to discuss parathyroid gland surgery. Also, Dr. Larian can help patients determine if parathyroid gland surgery is the best choice for treatment, along with performing an MIP that helps his patient alleviate HPT symptoms and prevent them from recurring.
If you would like to know more about the benefits of intra-operative PTH testing, or if you are considering an MIP, schedule a consultation with our parathyroid expert, Dr. Larian, by calling 310.461.0300 today!
