Minimally Invasive Parathyroidectomy (MIP) has a high cure rate, but the exact numbers depend on your surgeon’s experience. In fact, MIP’s success depends on the surgeon’s understanding of the disease, the technique used, how the surgeon assesses all 4 parathyroid glands’ function and level of expertise. Parathyroidectomy performed by surgeons that are inexperienced and do only a small number of parathyroid surgeries a year, have a much lower success rate (around 80-85% range), with much higher rate of complications and repeat surgeries. If MIP is performed by an experienced surgeon, cure rates are expected to be around 93-95%. At the CENTER for Advanced Parathyroid Surgery, our team has a MIP[1] cure rate of more than 97%.
When speaking of cure rates you have to talk separately about parathyroid adenoma and parathyroid hyperplasia. The symptoms and long term consequences of hyperparathyroidism caused by a parathyroid adenoma, or parathyroid hyperplasia are the same. However, the disease process is different, and the treatment (surgery) is different, consequently the discussion and explanation of cure rates are very different.
Parathyroid Adenoma Surgery Cure Rates
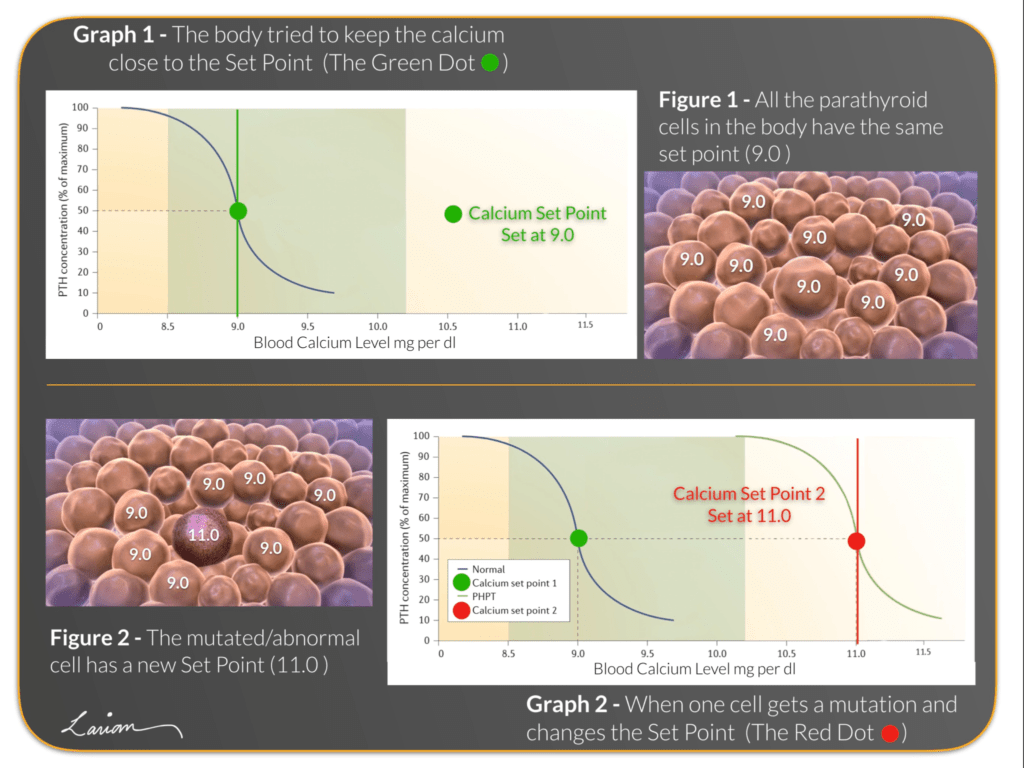
When a person has hyperparathyroidism due to a parathyroid adenoma, it is because there is a mutation in the calcium sensing mechanism (like a change in the thermostat setting), making the mutated parathyroid cell want a higher calcium level (for example: from a calcium of 9.0 to 11.0 – Graph 1 changes into Graph 2). As a consequence the abnormal parathyroid cell will need to be exposed to much higher levels of calcium before it is turned off and stops producing PTH. The mutated parathyroid adenoma cell that is trying to make the blood calcium level be higher, works hard to achieve this. In the process it keeps duplicating itself and getting bigger and bigger (dark blue cells in diagrams 2,3 & 4 – Figure 3).
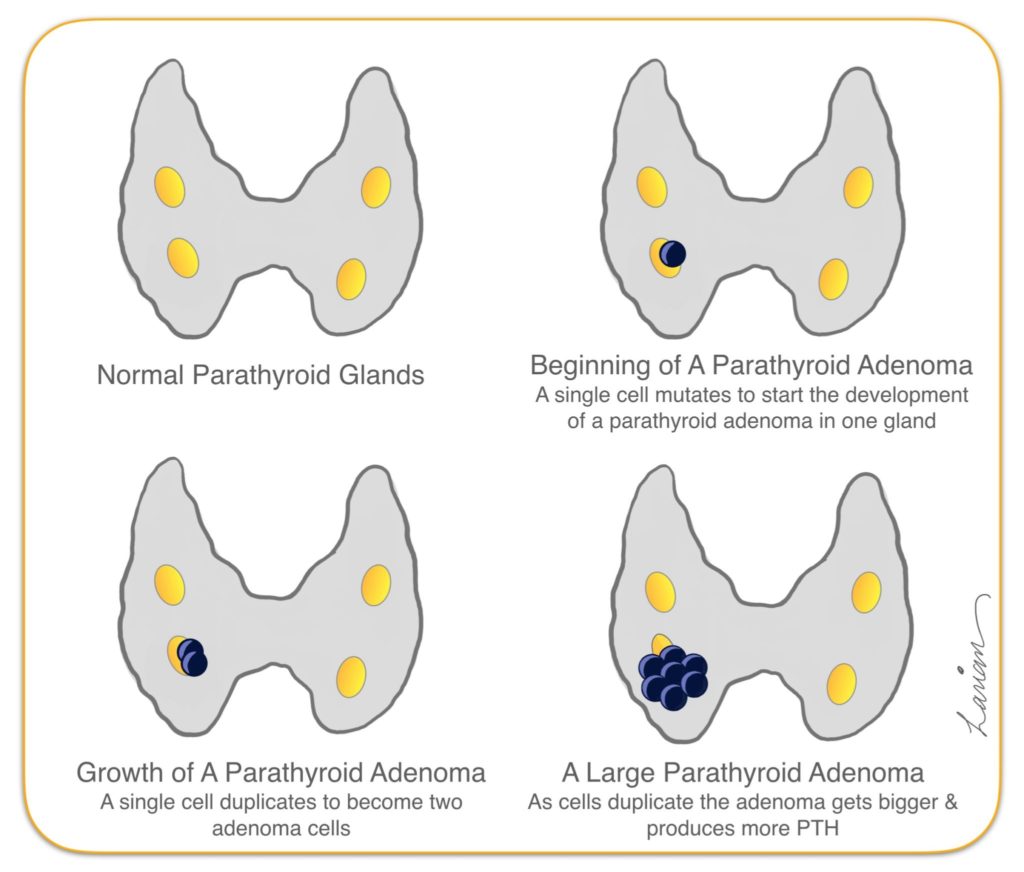
Once the blood tests confirm that the person has hyperparathyroidism, the next most important task for the surgeon is to identify which gland is the abnormal one by doing a scan or scans to find the parathyroid adenoma (at The CENTER we prefer ultrasound or 4D Parathyroid CT scan). Once the abnormal gland is identified, a minimally invasive parathyroidectomy is done with rapid intraoperative PTH testing to remove the abnormal gland, and make sure the remaining 3 glands are sleeping and producing very little PTH (PTH tested during surgery to show the other 3 glands are not over-active, and confirm the success of surgery before the patient wakes up).
When the surgery for parathyroid adenoma is done in this way the cure rates are more than 97%.
What is the reason to not get 100% cure rates for parathyroid adenoma?
This is a very important question. About 10% of people who have hyperparathyroidism have more than one parathyroid adenoma. Majority of times the second enlarged gland is identified when doing the localization scans (Ultrasound or 4D Parathyroid CT Scan). Sometimes the second parathyroid adenoma is not very big or may be in the very early stages of development. So small that it may not be visible to the surgeon’s eye in surgery, or visible on scans, and because at this small size it is not producing a significant amount of PTH, intraoperative-operative PTH testing may not show it (Fig 5). Unfortunately, these small parathyroids don’t show up on the sestamibi scan or radio guided surgery (MIRP) either (too small to be radioactive enough to be detected).
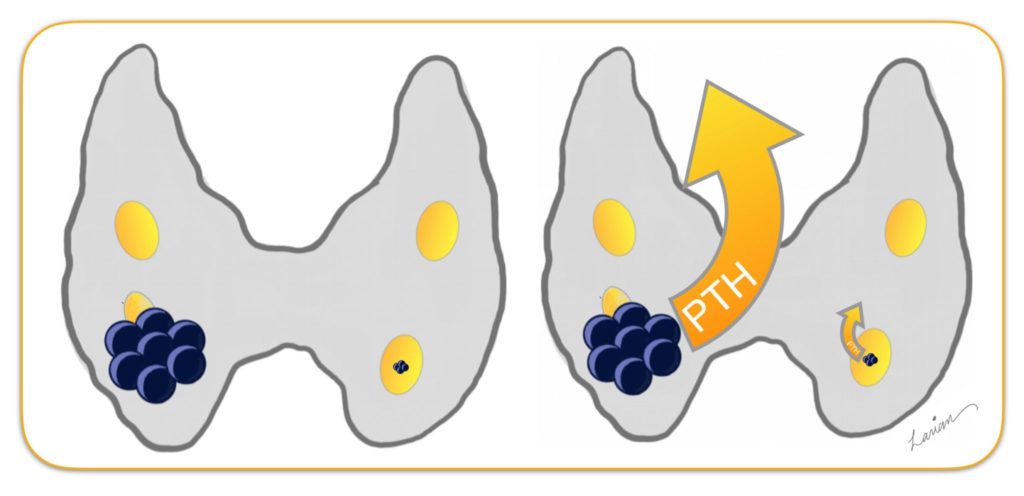
Another reason for not having a successful surgery is that the second adenoma may be small, not visible on scans and in an unusual location such as all the way up in the throat, or all the way down in the chest. This can occur because the parathyroids develop in the fetus (in the mother’s belly) from pouches that form in the throat. Once they have formed they migrate down to the neck and most of the time (80%) end up behind the thyroid (Figure 6. A ). However, sometimes they don’t travel enough to get to the thyroid (B), and at other times they move too much, pass the thyroid and go all the way down into the chest (C). We call these ECTOPIC PARATHYROIDS. Ectopic parathyroid glands that are small and not very active (making small amounts of PTH) will be missed on scans or MIRP.
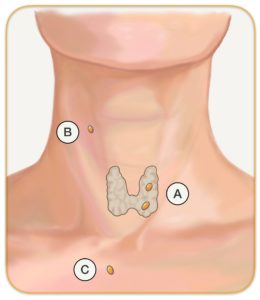
| Figure 6. While in the mother’s belly the parathyroid glands develop & migrates from throat to neck, & and can be in abnormal positions |
During surgery if the surgeon finds that after removal of one gland (that has parathyroid adenoma in it) the PTH has not come down enough, and therefore searches for the other 3 glands to see which one may appear abnormal (larger, rounder or darker coloration); finds 2 glands that are normal and the fourth gland is not present despite a comprehensive search. This probably means that the fourth gland has an adenoma, and is in an ectopic (unusual) position, that is out of the reach of the current surgical incision. And since the scan doesn’t see it, the surgeon=wouldn’t know where to look for it in the neck or chest. This is the second reason for surgery failing.
Despite these potential pitfalls, minimally invasive parathyroidectomy with intraoperative PTH testing has a more than 97% cure rate.
Parathyroid Hyperplasia Surgery Cure Rates
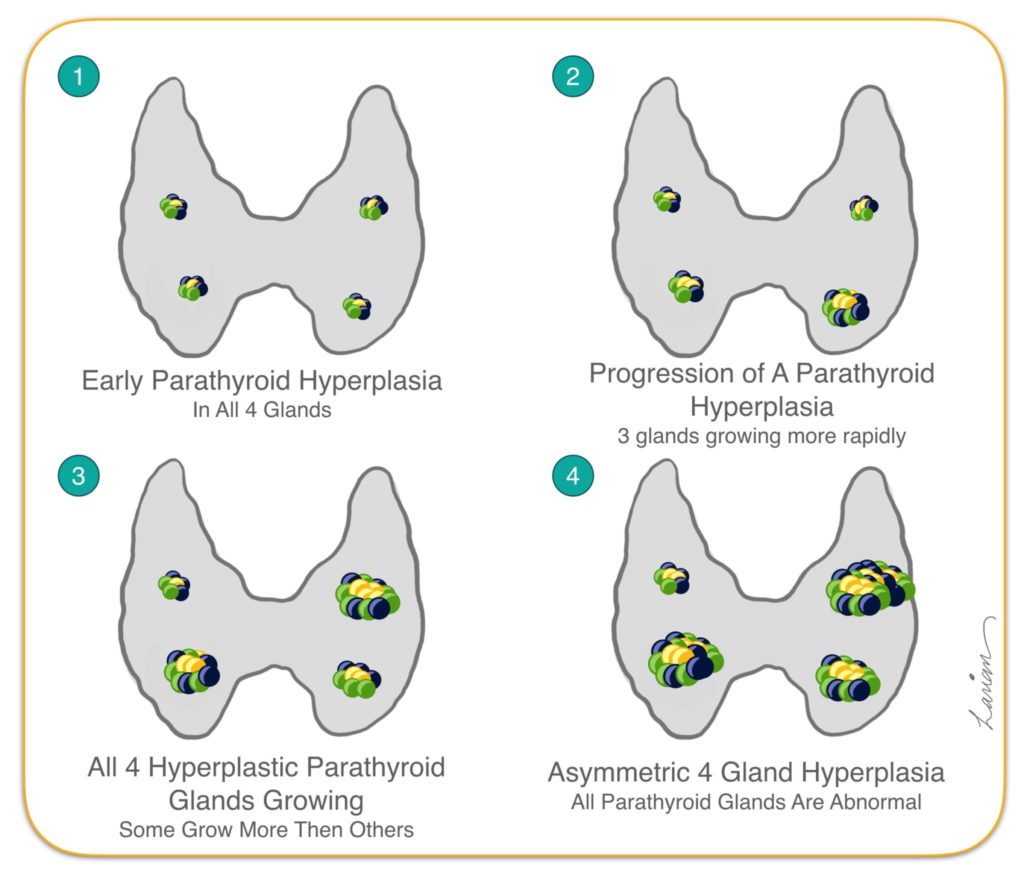
When a person has hyperparathyroidism due to 4 gland hyperplasia, this means not only all parathyroid glands are abnormal, but also all the cells in all 4 parathyroid glands are abnormal. Each parathyroid gland has roughly 5 millions cells within it. These cells have genetic mutations in them that cause them to continually grow (Figure 7). The rate of growth may be different for each of these glands, thus most often at the time of surgery one finds that each gland may be a different size. Some may have such a slow growth rate that they may appear normal.
The aim of surgery for hyperparathyroidism due to 4 gland hyperplasia is not to get rid of (or remove) all abnormal glands, but rather decrease the number of abnormal parathyroid cells to the point where the functionality is in the normal range. Basically the more abnormal parathyroid cells there are, the more PTH is produced above the needs of the body. So by reducing the number of abnormal cells in surgery the production of PTH is brought down to levels that meet the body’s needs.

There are 3 techniques to achieve this (Figure 8). Each of these techniques reduce the number of abnormal parathyroid cells while leaving a small portion of abnormal parathyroid behind; this usually means leaving a portion (50%-100%) of the smallest of the four parathyroid glands. The hope is that by doing this the parathyroid that is left behind is large enough to perform adequate calcium balancing; while at the same time taking a very long time to grow and become overactive again. In a great number of cases (greater than 90%) the time period it takes to grow and become overactive is so long that it does not occur in the person’s lifetime, in which case it is as if this person was cured.
Failure of parathyroid hyperplasia surgery is defined as persistent elevation of calcium or PTH immediately after surgery that continues over time, or re-occurrence of high numbers after a certain period of time. The reasons for failure are of parathyroid hyperplasia surgery are the following:
- Leaving too much of the 4th parathyroid gland behind. This happens because the surgeon has to make an estimation of how much parathyroid to leave behind so that the patient doesn’t develop permanent hypoparathyroidism, while at the same time not leaving too much of the 4th parathyroid gland that would cause hyperparathyroidism to still be present. This is where the experience of the surgeon is very helpful in getting the best results.
- Having more than 4 glands and not finding the extra (5th, 6th etc…) gland. The extranumerary gland (or the 5th gland or more) may be close to the other glands and easily identified or maybe farther away in the chest or throat and not be accessible. Having access to reliable localization studies is very helpful in these circumstances.
Parathyroidectomy Cure Rates FAQ
If a person has a successful parathyroid adenoma surgery, what are the chances that they may get hyperparathyroidism years later?
Very important question, there are reports that anywhere between 3-10% lifetime chance of developing another parathyroid adenoma. The reason for this is that whatever environmental toxin caused the first adenoma to develop has not been identified, and the person can’t prevent exposure to it. As such there is the possibility that the person is still exposed and may develop another adenoma. Fortunately this chance is low. Due to this we recommend that after surgery all patients do a yearly calcium, PTH, and vitamin D blood tests.
This is also the reason our philosophy is to perform minimally invasive parathyroidectomy that focuses on surgery on one gland and confirmation with intraoperative-operative PTH testing; this way the other gland areas are not violated during the original surgery so that if the person gets another adenoma years later, there will be minimal scarring and the risk of repeat surgery will be significantly less.
Is the cure rate lower for people who have hyperparathyroidism run in their family?
If they have an adenoma then the cure rate is the same, however the chance of parathyroid hyperplasia is higher when there is a family history of hyperparathyroidism. The surgeon has to take this into consideration before and at the time of surgery.
Does the size of the parathyroid adenoma affect the cure rate?
Yes, the larger the parathyroid adenoma the easier it is to find it on localization scans, and during surgery.
Does the PTH level affect the chance of finding the abnormal gland?
The size of the abnormal parathyroid gland directly correlates the PTH level, so the higher the PTH level the larger the parathyroid adenoma. The larger the gland the easier it is to find by scans and during surgery.
How can a person know that they have hyperplasia before going to the operating room?
The only people that know that they have hyperplasia are the ones that have either familial hyperparathyroidism where all the other members have had hyperplasia (MEN 1 syndrome), or if they have secondary hyperparathyroidism due to kidney failure. In all other circumstances there is no way to be certain. However, we also know that when the PTH levels are high (greater than 150 pg/ml) the chances of hyperplasia is around 5%. And when the PTH is less than 100 pg/ml then the chance is significantly more.









